Wednesday, December 22, 2010
Relapse Concerns
Monday, December 20, 2010
Breastfeeding a Triangle

Breastfeeding with leg braces on is an art form... but with pillows and some patience anyone can do it! :)
Thursday, December 16, 2010
Two Weeks in Braces
Side Sleepers



Monday, December 13, 2010
Giant Clothing Pity Party

Let me start this post off by saying do not feel like I am ungrateful for gifts we have received. Many of these I probably registered for before we knew that our children had clubbed feet. Why would someone ever think their child would be unable to wear a certain article of clothing?? Right?
Tuesday, December 7, 2010
First Week In Braces

 Since my post last week my daughters toes have curled even more! Now the 3rd, 4th, and 5th toes are all curling under. I have a feeling that the casting was holding the 3rd & 4th toes up and now that the cast isn't there anymore they are free to curl. The surgery to correct this is a tenotomy of the tendons in the toe/foot. They are too tight and are causing the toes to curl down permanently.
Since my post last week my daughters toes have curled even more! Now the 3rd, 4th, and 5th toes are all curling under. I have a feeling that the casting was holding the 3rd & 4th toes up and now that the cast isn't there anymore they are free to curl. The surgery to correct this is a tenotomy of the tendons in the toe/foot. They are too tight and are causing the toes to curl down permanently.
 using the rubber insert... but I think it was meant for a baby much bigger than ours.
using the rubber insert... but I think it was meant for a baby much bigger than ours.Sunday, December 5, 2010
Ponseti Method
This is straight up copy/pasted from Wikipedia. I know, I'm lame this week... Ha!
Ponseti treatment was introduced in UK in the late 1990s and widely popularized around the country by NHS physiotherapist Steve Wildon. The manipulative treatment of clubfoot deformity is based on the inherent properties of the connective tissue, cartilage, and bone, which respond to the proper mechanical stimuli created by the gradual reduction of the deformity. The ligaments, joint capsules, and tendons are stretched under gentle manipulations. A plaster cast is applied after each manipulation to retain the degree of correction and soften the ligaments. The displaced bones are thus gradually brought into the correct alignment with their joint surfaces progressively remodeled yet maintaining congruency. After two months of manipulation and casting the foot appears slightly over-corrected. After a few weeks in splints however, the foot looks normal.
Proper foot manipulations require a thorough understanding of the anatomy and kinematics of the normal foot and of the deviations of the tarsal bones in the clubfoot. Poorly conducted manipulations will further complicate the clubfoot deformity. The non-operative treatment will succeed better if it is started a few days or weeks after birth and if the orthopedist understands the nature of the deformity and possesses manipulative skill and expertise in plaster-cast applications.[2]
Clubfoot (talipes equinovarus) affects almost 150,000 children annually. Almost 80% of these children live in developing nations. Dr Ponseti's technique is painless, fast, cost-effective and successful in almost 100% of all congenital clubfoot cases. The Ponseti method is endorsed and supported by World Health Organization [3], National Institutes of Health[4], American Academy of Orthopedic Surgeons [5], Pediatric Orthopedic Society of North America [6], European Pediatric Orthopedic Society [7], CURE [8], STEPS Charity UK [9], STEPS Charity South Africa [10], A Leg to Stand On (India) [11] and others.
At the 2007 International Clubfoot Symposium attended by 200 doctors from 44 countries, papers were presented for an estimated 10,000 children successfully treated with the technique around the world in the past few years.
The Ponseti International Association for the Advancement of Clubfoot Treatment was founded in 2006 at the University of Iowa. The Ponseti International Association aims to improve the treatment of children born with clubfoot through education, research and improved access to care.
Steps are as follows:
1. The calcaneal internal rotation (adduction) and plantar flexion is the key deformity. The foot is adducted and planter-flexed at the subtalar joint, and the goal is to abduct the foot and dorsiflex it. In order to achieve correction of the clubfoot, the calcaneum should be allowed to rotate freely under the talus, which also is free to rotate in the ankle mortise. The correction takes place through the normal arc of the subtalar joint. This is achieved by placing the index finger of the operator on the medial malleolus to stabilize the leg and levering on the thumb placed on the lateral aspect head of the talus while abducting the forefoot in supination. Forcible attempts at correcting the heel varus by abducting the forefoot while applying counter pressure at the calcaneocuboid joint prevents the calcaneum from abducting and therefore everting.
2. Foot cavus increases when the forefoot is pronated. If cavus is present, the first step in the manipulation process is to supinate the forefoot by gently lifting the dropped first metatarsal to correct the cavus. Once the cavus is corrected, the forefoot can be abducted as outlined in step 1.
3. Pronation of the foot also causes the calcaneum to jam under the talus. The calcaneum cannot rotate and stays in varus. The cavus increases as outlined in step 2. This results in a bean-shaped foot. At the end of step 1, the foot is maximally abducted but never pronated.
4. The manipulation is carried out in the cast room, with the baby having been fed just prior to the treatment or even during the treatment. After the foot is manipulated, a long leg cast is applied to hold the correction. Initially, the short leg component is applied. The cast should be snug with minimal but adequate padding. The authors paint or spray the limb with tincture of benzoin to allow adherence of the padding to the limb. The authors prefer to apply additional padding strips along the medial and lateral borders to facilitate safe removal of the cast with a cast saw. The cast must incorporate the toes right up to the tips but not squeeze the toes or obliterate the transverse arch. The cast is molded to contour around the heel while abducting the forefoot against counter pressure on the lateral aspect of the head of the talus. The knee is flexed to 90° for the long leg component of the cast. The parents can soak these casts for 30–45 minutes prior to removal with a plaster knife. The authors' preferred method is to use the oscillating plaster saw for cast removal. The cast is bivalved and removed. The cast then is reconstituted by coapting the 2 halves. This allows for monitoring of the progress of the forefoot abduction and, in the later stages, the amount of dorsiflexion or equinus correction.
5. Forcible correction of the equinus (and cavus) by dorsiflexion against a tight Achilles tendon results in a spurious correction through a break in the midfoot, resulting in a rockerbottom foot. The cavus should be separately treated as outlined in step 2, and the equinus should be corrected without causing a midfoot break. It generally takes up to 4-7 casts to achieve maximum foot abduction. The casts are changed weekly. The foot abduction (correction) can be considered adequate when the thigh-foot axis is 60°After maximal foot abduction is obtained, most cases require a percutaneous Achilles tenotomy. This is performed in the cast room under aseptic conditions. The local area is anesthetized with a combination of a topical lignocaine preparation (eg, EMLA cream) and minimal local infiltration of lidocaine. The tenotomy is performed through a stab incision with a round tip (#6400) Beaver blade. The wound is closed with a single absorbable suture or with adhesive strips.The final cast is applied with the foot in maximum dorsiflexion, and the foot is held in the cast for 2–3 weeks.
6. Following the manipulation and casting phase, the feet are fitted with open-toed straight-laced shoes attached to a Dennis Brown bar. The affected foot is abducted (externally rotated) to 70° with the unaffected foot set at 45° of abduction. The shoes also have a heel counter bumper to prevent the heel from slipping out of the shoe. The shoes are worn for 23 hours a day for 3 months and are worn at night and during naps for up to 3 years.
7. In 10-30% of cases, a tibialis anterior tendon transfer to the lateral cuneiform is performed when the child is approximately 3 years of age. This gives lasting correction of the forefoot, preventing metatarsus adductus and foot inversion. This procedure is indicated in a child aged 2–2.5 years with dynamic supination of the foot. Prior to surgery, cast the foot in a long leg cast for a few weeks to regain the correction.
Wednesday, December 1, 2010
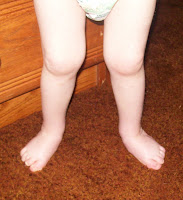
Woes about Toes
 Our son has what they call "curly toes" where the middle toe is too low and it's pushing up on the toe next to it. He was born with the right one that way, and through correcting his clubbed feet the left has also crossed. It is possible that over the next few months they will fix themselves as his feet move into neutral positioning, but if not... we may be headed for a minor surgery. They will simply release the tendon that is holding the middle toe too low and then things should align naturally. We've battled whether this is cosmetic surgery or not, and it is something we will talk about extensively before agreeing to surgery. It is my feeling that this would be mighty uncomfortable in shoes as his feet grow.
Our son has what they call "curly toes" where the middle toe is too low and it's pushing up on the toe next to it. He was born with the right one that way, and through correcting his clubbed feet the left has also crossed. It is possible that over the next few months they will fix themselves as his feet move into neutral positioning, but if not... we may be headed for a minor surgery. They will simply release the tendon that is holding the middle toe too low and then things should align naturally. We've battled whether this is cosmetic surgery or not, and it is something we will talk about extensively before agreeing to surgery. It is my feeling that this would be mighty uncomfortable in shoes as his feet grow.
Tuesday, November 30, 2010
6th & Final week of casting...?

Well, today was full of surprises. We went in for our 6th cast removal, fully assuming that we'd be getting a tenotomy afterwards and then having 2-3 additional weeks of casting after that. I was even more sure that it was going to happen since our doctor, who normally wears a suit, walked into the exam room in operating room scrubs and he had two assistants with him. He examined her feet, stretching them as far as they could be forced. He said it could get her to about 20 degrees up, and that ideally he'd like to see 25 degrees - but that ultimately he wasn't sure that just doing physical therapy (the "french method" he called it) of stretching her daily wouldn't work just as well as the surgery to get that extra 5 degrees. So, for now, we are holding off on the tenotomy and have 5 weeks to see if we can manually stretch her feet. Fingers crossed!!


 a little bit, so the heel was raw from rubbing on the shoe. :( Oops. I've made them tighter now and she hasn't done much complaining since then.
a little bit, so the heel was raw from rubbing on the shoe. :( Oops. I've made them tighter now and she hasn't done much complaining since then.Thursday, November 25, 2010
Tenotomy

Club foot is a common developmental deformity in which the foot is turned inward, with shortening of one or more of the muscles controlling the foot and possibly some bone deformity as well.
A muscle can become shortened and resistant to stretch when it remains in a shortened position for many months. When this occurs, the tendon that attaches muscle to bone can shorten, and the muscle itself can develop fibrous tissue within it, preventing it from stretching to its full range of motion. This combination of changes is called contracture.
During a tenotomy, the tendon is cut entirely or partway through, allowing the muscle to be stretched. Tenotomy may be performed through the skin (percutaneous tenotomy) or by surgically exposing the tendon (open tenotomy). The details of the operation differ for each tendon.
During a percutaneous lengthening of the Achilles tendon, a thin blade is inserted through the skin to partially sever the tendon in two or more places. This procedure is called a Z-plasty, and is very rapid, requiring only a few minutes. It may be performed under local anesthesia.
Tenotomy carries a small risk of excess bleeding and infection. Tenotomy performed under general anesthesia carries additional risks associated with the anesthesia itself.After tenotomy, the patient may receive pain medication. This may range from over-the-counter aspirin to intravenous morphine, depending on the severity of the pain. Ice packs may also be applied. The patient will usually spend the night in the hospital, especially children with swallowing or seizure disorders, who need to be monitored closely after anesthesia.
Casts are applied to the limb receiving the surgery. Before the cast is applied, the contracted muscle is stretched to its normal or near-normal extension. The cast then holds it in that position while the tendon regrows at its extended length. Braces or splints may also be applied.
After the casts come off (typically two to three weeks), intensive physical therapy is prescribed to strengthen the muscle and keep it stretched out.
Properly performed, tenotomy does not carry the risk of mortality. It may cause temporary pain and bleeding, but these are usually easily managed.Reference: http://www.surgeryencyclopedia.com/St-Wr/Tenotomy.html
Wednesday, November 24, 2010
5 Weeks In...
Monday, November 22, 2010
Support Groups
Friday, November 19, 2010
Celebrities Born with Clubbed Feet
Monday, November 15, 2010
4 Weeks In...

Well, todays appointment raised my blood pressure a little bit. Sometimes it's hard to be going through this a second time because the medical staff assumes that I am old hat at it, but we must remember that I had it pretty "easy" with my son and everything was 'best case scenario' with his recovery.


Wednesday, November 10, 2010
Comfort Measures - TIPS & TRICKS

Casted legs are heavy and pull on the hips when a baby is sleeping on their back. Rolling up a towel and putting it under the knees helps take some of the pressure off and hopefully help baby sleep better. I've also seen parents do this in the car seat if the angle seems to be too steep to let the legs rest easily.

Monday, November 8, 2010
3 Weeks In...
Bye, Bye casting room......

Sunday, November 7, 2010
Decorate - TIPS & TRICKS



Make casting fun! Decorate them... have friends sign it every week... let older siblings color on them... crochet little leggings... tons of ideas to make the process a little brighter. :)
Saturday, November 6, 2010
Odd Sized Shoes - TIPS & TRICKS
When all is said and done for clubbed foot babies sometimes their feet are different sizes. My son's are about a 1/2 size off from each other, but we just wear the same size. I know some children have a bigger difference and need buy two pairs of the same shoes to get the right sizes or find places that will let you order different sizes. I found these places can help parents like those of us with different foot sizes by providing mix matched shoes.
Hope these help some of you too.
Wednesday, November 3, 2010
$h*t Happens

Sigh. No matter how careful you are... at some point in the casting process... it... will... happen. Babies poop a lot and it's only a matter of time before some get on the casts. We're 16 days into her recovery and shockingly have been able to stay poop free until this point.
Tuesday, November 2, 2010
Two Week Appointment


We had our appointment this morning to change out baby girls casts. We were hopeful that today would be the end of casting... but it looks like one more week is our destiny. Her feet aren't quite in the "L" shape yet. Fingers crossed that this is the last week!
 long. She tucked some extra cotton into the fold this week
long. She tucked some extra cotton into the fold this weekMonday, November 1, 2010
Gassy Baby - TIPS & TRICKS
Wednesday, October 27, 2010
Emotions

Tuesday, October 26, 2010
One Week into Recovery


My baby girl has been in casts for a full week. Her ankles are already straight! What a big improvement. I've had many questions about what the casts do, and the basic answer is that they help align the calves and ankles to be straight. It holds her legs in position and helps stretch out the tendon that has her legs curling. There is a science behind what angle her legs are held in. When she moves into the Ponseti bar braces they will be angling her feet into the correct position. Actually, they OVER correct because once she is out of the brace there will always be a period where the feet start to turn back inward. Yearly follow up appointments will make sure her feet are on track. So, casts take care of the legs and the braces take care of the feet. That is my understanding of it anyway!
Saturday, October 23, 2010
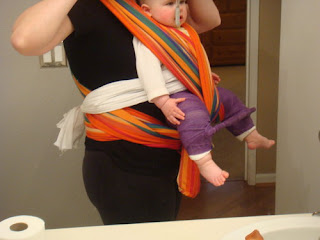
Babywearing with Spica Cast
I used a woven wrap and faced out because of the bar on the spica cast. The spica cast keeps the hips in the proper position. Without it, you have to be very careful to make sure the rails are under the legs, and supporting your DD in a seated position. Since it is not as bulky as the spica cast you might be able to use the Pikkolo or Gemini. Those are buckle carriers that can face out in a seated position. Most of the forward facing carriers are pretty bad. I know you can rent them from PaxBaby. Jillian is very sweet and would be glad to help you out. I do have to warn that you need to watch out for overstimulation when forward facing. Jilly used to get pretty fussy if we were in a busy place too long because there was no place ti hide her head and get away from it all.
Steps to wrapping:
1. Safety pin the wrap in 2 places in the back to keep it in place.
2. Pick up the baby and thread the wrap up through the bar and over the shoulders. Make sure it is tight and baby is close up against the body. The straps should be in an X across the front.
3. Cross the straps around the back, in an X across your back. Tighten thoroughly.
4. Bring the straps under the baby's bottom and tie the wrap.
5. Spread the wrap so that it is supporting baby's bottom and back well.
6. Thread a strip of cotton gauze through the center of the wrap and tie it around the baby and yourself to add support to the sides.
Here is a video of the type of wrap I am basing this on.
http://www.gypsymama.com/beginner.htm#x

Here are 2 other techniques using the Front Wrap Cross Carry. Both eliminate the need for an extra peice of fabric or safety pins.
http://www.wrapyourbaby.com/frontwrapcrosscarry.htm
Both techniques start with finding the middle of the wrap and holding it up to your chest then bringing the rails over the opposite shoulder.
The first technique has DD facing out like the above technique.
1. Instead of making a pouch, the piece of the wrap around your chest is used as cumberbund. It must be left pretty loose to get the baby in there, and the baby will be facing out instead of in.
2. Then tug on the rails to tighten the cumberbundt securely around your babies middle.
3. Thread one rail through the bar of the cast, downward and spread it across your baby's bottom for support. The rails will make an X.
4. Bring the second rail down thorugh the bar and spread evenly.
5. Bring the rails around your back and tie them off.